Top Strategies for Improving Patient Collections (2026 Ultimate Guide)

Top Strategies for Improving Patient Collections (2026 Guide) As we navigate 2026, the financial burden on patients has reached an all-time high. For the modern medical practice, patient collections are no longer a “back-office” task—they are a front-line necessity. Without an optimized strategy, small practices are currently losing an average of 15-20% of their net […]
What Is Charge Posting In Medical Billing?
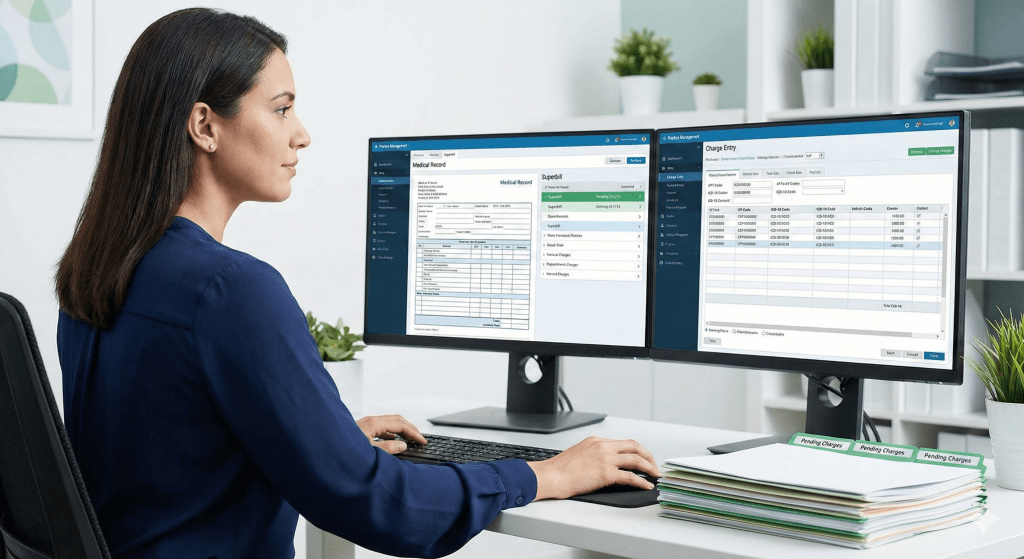
Behind every successful medical practice is a highly accurate billing system. But before an insurance company pays you a single dollar, there is one critical step that dictates your entire cash flow: Charge Posting. If you get this wrong, your practice bleeds revenue. Here is everything you need to know about the most important phase […]
7 Practical Tips for Small Practices for Quick AR Recovery

Accounts Receivable (AR) is the financial lifeblood of your private practice. If your claims are aging past 45 days, your cash flow is actively depreciating. According to the Medical Group Management Association (MGMA), the average small practice leaves up to 15% of its total revenue on the table due to unworked aging AR. Here is […]
Do Nurses Have NPI Numbers? The 2026 Requirement Guide
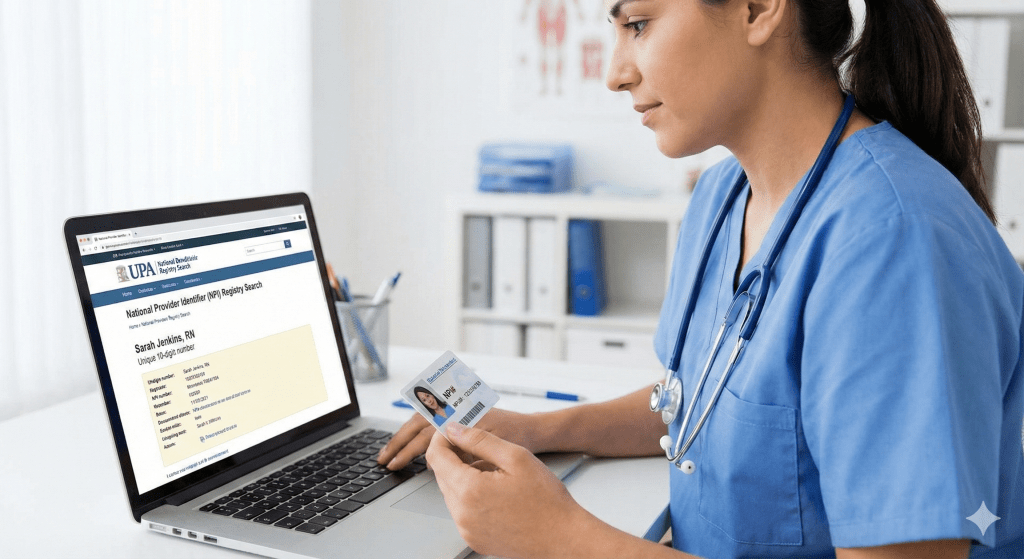
Provider Enrollment Series | Updated for 2026 The Short Answer Does a nurse need an NPI? It depends entirely on their role. Nurse Practitioners (NPs), Midwives (CNMs), and CRNAs must have one to bill insurance. Registered Nurses (RNs) generally do not need one unless they work in specialized fields like Home Health or Case Management. […]
What is Explanation of Benefits (EOB) in Medical Billing?

Revenue Cycle Education | Updated for 2026 Standards The Short Answer An Explanation of Benefits (EOB) is a statement sent by a health insurance company to a patient explaining what medical treatments were paid for on their behalf. It is not a bill. It clarifies the “Allowed Amount,” what the insurance covered, and the “Patient […]
How to See Patients When the Physician Isn’t Credentialed Yet? (2026 Strategies)

A Definitive Guide to Bridging the “Revenue Gap” | Written by Adam Blake • 2 Minute Read The Cost of the “Credentialing Gap” You have hired a brilliant new physician. They have started work. Patients are scheduled. But their insurance credentialing is still “Pending.” This 90-120 day gap is the “Credentialing Limbo,” and without a […]
What are the best Insurance Panels for Therapists?

A Strategic Ranking for Private Practice Growth | Written by Adam Blake The Quick Verdict For most private practice therapists, Blue Cross Blue Shield (BCBS) offers the best balance of high reimbursement rates and patient volume. UnitedHealthcare (Optum) is essential for volume, and Aetna is the leader in telehealth support. The “Cash-Pay vs. Insurance” debate […]
Credentialing With Medicaid: A Comprehensive Guide (2026)

The “Volume Engine” of Private Practice | Written by Adam Blake What is Medicaid Credentialing? Medicaid credentialing is the formal process of enrolling as a provider with state-funded health programs. Unlike Medicare (which is federal), Medicaid is run by individual states. This means there are 50 different application processes, often involving a complex web of […]
HCPCS Code J3490: Complete Guide to Unclassified Injectable Drug Billing (2026)

Updated for 2026 Payer Standards | Written by Adam Blake What is J3490? HCPCS J3490 is a miscellaneous billing code used for injectable drugs that have been FDA-approved but do not yet have a specific code assigned. It allows providers to bill for new or “unclassified” drugs immediately, rather than waiting for the quarterly CMS […]
How Much Time Does Credentialing a Provider Take in 2026?

Updated for 2026 Payer Standards | Written by Adam Blake The Executive Summary In 2026, the medical credentialing process typically takes between 90 to 120 days for commercial payers (Aetna, Cigna, BCBS) and 30 to 60 days for Medicare. However, timelines can extend up to 150 days if there are errors in the application, gaps […]
